Single lung ventilation, also known as 'One Lung' ventilation, is a method of ventilation which was first conceptualized by physiologists Eduard Pflüger and Claude Bernard who studied gas exchange in dogs using a lung isolation catheter.The first instance of clinical use in humans was by Loewy and VonSchrotter with lower lobe bronchus catheterized under fluoroscopic control. Gale and Walters in 1932 advanced Head's design and created the prototype for the modern day double lumen tubes. Double lumen tubes paved the way for one-lung ventilation offering better control of ventilation and more efficient separation of the two lungs.
Single lung ventilation involves ventilating one lung and letting the other collapse for providing surgical exposure in the thoracic cavity or isolating ventilation to one lung. The protective role of the single lung ventilation involves protecting one lung from the ill effects of fluid from the other lung - which may be blood, lavage fluid, malignant or purulent secretions. Thus it is prudent to ensure perfect placement of the tube as a misplaced tube defeats the goals of lung isolation or differential ventilation. This is ensured by bronchoscopy done after tube placement and after any position changes thereafter.
The indications of single lung ventilation aim at facilitating surgical exposure by isolating the lung away from the field of surgery or preventing further lung trauma by providing selective ventilation as well as preventing infection or secretions from entering the healthy lung. They include video-assisted thoracoscopic surgery including pneumonectomy, wedge resections, pulmonary resections including pneumectomies and lobectomies, mediastinal surgery, thoracic vascular surgery, oesophageal surgery, spine surgery and protective lung isolation in massive pulmonary haemorrhage or infection/purulent secretions.
However, there are some relative contraindications for single lung ventilation. For instance in cases where patient is unable to tolerate OLV/Dependence on bilateral ventilation, intraluminal airway masses (making DLT placement difficult), hemodynamic instability, severe hypoxia, severe COPD, severe pulmonary hypertension or known or suspected difficult intubation.
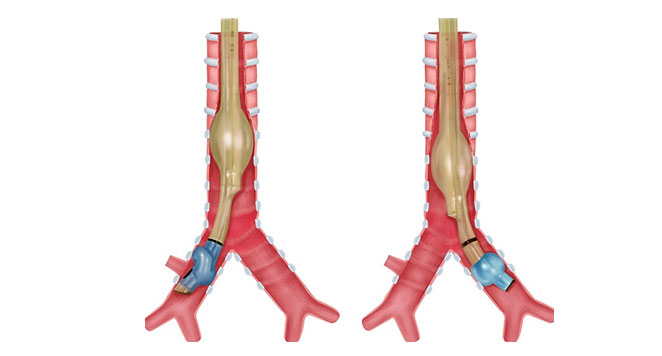
Single lung ventilation is achieved with the use of special airway devices such as double lumen tubes (DLT) and bronchial blockers (BB) which selectively direct the airflow to one lung. They are used to collapse one lung selectively for surgery on the ipsilateral side.
Patients usually undergoing single lung ventilation for a variety of procedures have underlying pulmonary disease. Patients should be evaluated comprehensively for their primary disease prior to performing the surgical procedure. Echocardiography may be useful in patients with cor pulmonale and may provide information about baseline cardiac function and reserve.
Single lung ventilation aims at two separate goals - to maintain adequate oxygenation and to maintain lung isolation and lung protection. The challenges faced by an anaesthesiologist in performing one lung ventilation arise from a combination of lateral decubitus positioning, open pneumothorax, and the anaesthetic technique. The lateral decubitus position brings about physiological changes in the ventilation-perfusion matching, and this is subsequently altered under anaesthesia by the effects of neuromuscular blockade, open thorax, hypoxic pulmonary vasoconstriction, surgical retraction, differential blood flow to the dependent and the non-dependent lungs.